Physiotherapists stay in the slipstream in between feature and feeling. We work to bring back movement, yes, yet every strategy hinges on whether a person can endure the trip. Pain flexes pose, disrupts sleep, misshapes motor control, and can gut a promising recovery program. That is why formal pain administration training, and particularly the national unit PUAEME008 Provide pain administration, should have a clear description from a physical rehabilitation perspective. Many medical professionals listen to the code, know it relates to prehospital and emergency contexts, and question just how it equates to daily method. The brief answer: it includes a solid, safety-focused layer to your medical ability, particularly for acute pain situations, urgent treatment setups, outreach work, and multidisciplinary atmospheres where prompt analgesia and organized assessment matter.
Where PUAEME008 fits in the landscape of pain education
Pain administration courses been available in many tastes. Some target the biopsychosocial approaches underpinning consistent discomfort. Others focus on pharmacology and administration, frequently designed for nursing or paramedical team. Then there are brief programs suffering administration that focus securely on severe discussions: musculoskeletal trauma, postoperative discomfort in area setups, or extreme flare-ups of chronic conditions. PUAEME008 beings in that last team. It is a functional, competency-based unit developed around the secure shipment of short-term analgesia within defined methods, coupled with structured analysis, documentation, and escalation.
For physiotherapists who supply treatment in urgent treatment, sporting activities sideline settings, area and rural outreach, or incorporated primary care hubs, the system pairs well with core physio abilities. It does not replace a certificate program suffering management that discovers main sensitization or inspirational speaking with, and it is not an alternative to a comprehensive discomfort monitoring certification that extends months. It is a focused credential that enhances sharp pain decision-making under scientific governance.
What "give discomfort administration" suggests in this context
PUAEME008 Supply discomfort management includes three pillars: evaluation, intervention within extent, and evaluation with documents. Evaluation is not just a 0 to 10 numeric score. It asks you to gather device, red flags, comorbidities, allergic reactions, and possible medication communications, after that determine if on-the-spot analgesia is suitable or if you require to escalate to healthcare. Treatments covered commonly focus on accepted, protocol-driven alternatives like breathed in analgesia or oral representatives allowed in your jurisdiction and work environment policies. The analysis item is extensive: reassess discomfort at specified intervals, observe for unfavorable effects, and document to ensure that the following medical professional obtains a clean handover.
Physiotherapists are normally educated to think activity initially. In the acute setting, activity rests on pain tolerability and safety. With PUAEME008, you are trained to determine, within your extent and neighborhood consent, whether temporary analgesia assists you do a safer assessment, minimize distress, and facilitate transport or referral. The system likewise hones your judgment regarding when not to provide analgesia, such as in presumed stomach emergencies needing surgical testimonial or in head injury where altered psychological status clouds the picture.
What the unit commonly covers
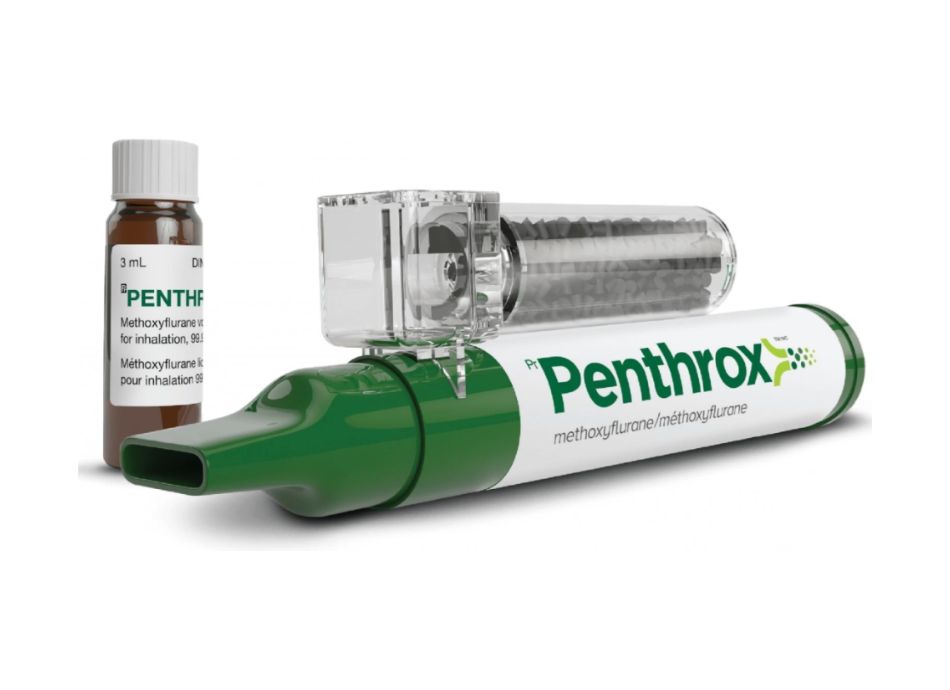
The specifics differ by provider, yet a strong pain management course aligned to PUAEME008 shares usual strings: fundamental pain science, danger testing, pharmacology basics appropriate to frontline care, non-pharmacological methods you can carry out instantly, and robust procedures for documents and handover. The training generally includes simulated circumstances with time pressure and insufficient details, which mirrors real-life problems remarkably well. You can anticipate skill terminals on breathed in analgesia if permitted in your area, useful opioid safety conversations, and acknowledgment of adverse reactions like hypotension, breathing anxiety, or paradoxical agitation.
A well-run program will stress systems assuming. Discomfort administration training is not almost the medicine; it is about radios that work, kit checks that catch running out cylinders, and constant auditing that closes safety and security loopholes. As a physiotherapist, you will certainly identify the alongside taping tables checked prior to sporting pain management courses for nurses activity, or drive tests standardized for inter-rater integrity. PUAEME008 is that mindset, related to severe pain.
Why physiotherapists benefit
Pain is the rate-limiting factor in numerous physiotherapy pathways. Intense side ankle joint strains, rib contusions, spinal flare-ups, adhesive capsulitis during severe stages, and post-fracture rigidity all test the individual's limit. In team sports and area emergencies, you might be the senior medical professional on scene. Structured training allows you to maintain, soothe pain safely, and refer with clean documentation. In facilities that sustain post-surgical people, the ability to identify poorly managed pain early, readjust non-pharmacological measures, and rise or liaise with medical coworkers can avoid issues like activity evasion and readmission.

I remember a Saturday morning clinic in a country town, where the nearby immediate treatment was an hour away. A ranch worker arrived with a believed rib crack after being smashed briefly by a gateway. Without training, the default would have been to incapacitate and send him on. With pain monitoring training and appropriate methods in place, we utilized a short-acting inhaled agent, monitored him very closely, and boosted his ventilation enough to reduce splinting. That made transport much safer and his distress manageable. The distinction was not heroic medicine, it was procedures carried out properly.
Comparing training course kinds for various clinicians
Physiotherapists frequently share discovering rooms with registered nurses and paramedics suffering monitoring training programs. The diversity assists. Registered nurses bring deep medicine safety experience, while physios add mechanical evaluation and movement-focused strategies. The overlap honed in the device improves interprofessional interaction. Discomfort administration training for nurses might lean a lot more on medication handling and administration policy. Discomfort monitoring programs for physiotherapists frequently stress evaluation connected to operate, bracing placements, and prompt activity approaches that reduce nociception. When mixed associates learn together, they merge on certificate course in pain management a common language of danger and reaction, which carries right into day-to-day collaboration.
For those who desire wider depth, a pain management certification course or a longer certification course suffering administration can check out persistent pain neurobiology, rated exposure, cognitive strategies, and case-coordination. Short programs hurting management, consisting of PUAEME008, fit best when you require to sharpen emergency discomfort management and severe decision-making.
Scope, consent, and the truth of practice
A bottom line: PUAEME008 Provide discomfort administration is not a freebie to carry out anything you such as. Extent continues to be linked to regulations and company policy. Even within protocol-based authority, you will certainly be assisted by incorporation and exemption criteria, dosage ranges, tracking requirements, and compulsory coverage. Prior to you book, check whether your method setting authorizes non-medical clinicians to give details agents. Private centers might need a standing order or clinical governance. Sporting companies may already have a policy structure for match-day protection. Community health services commonly have actually established medicine registers and audit pathways.
The best service providers of discomfort administration training programs will certainly inquire about your setting and dressmaker useful parts to what you can really carry out. If you can not carry out breathed in analgesia where you work, you can still get from advanced evaluation drills, non-pharmacological devices, and acceleration preparation. The certificate you get ought to mirror the proficiencies you were analyzed versus, not hypothetical permissions.
Core abilities the system sharpens
Pain analysis relocates past asking how poor it is. With the unit, you find out to triangulate intensity with effect, pattern, and red flag screens. Device overviews uncertainty. An inversion injury with a high-grade sprain offers in different ways to a midfoot injury where you could need to dismiss a Lisfranc injury. Rib discomfort with crepitus and shallow breathing increases worries about pneumonia threat if splinting continues. A clean discomfort monitoring certification shows that you can link this thinking to prompt actions, not just chart notes.
You will additionally practice titration and reassessment. Several analgesic choices work best when you supply the tiniest reliable dose, then reassess right away. The program trains you to mark time factors, capture vital signs, and support pain adjustments to functional end results like improved stride or capacity to take a full breath. That functional lens is where physio therapists succeed, and the device gives you language to record modifications with precision.
Non-pharmacological devices remain central
Even in an offer discomfort monitoring program, the non-drug methods project. Positioning can de-load short-tempered tissues in seconds. A client with severe back discomfort might tolerate side-lying with mild hip and knee flexion much better than supine. Gentle isometrics for the potter's wheel cuff can moisten pain with spinal-level gating. Ice or warm still have a place, but only when client choice and tissue state align. For rib trauma, we frequently integrate lateral costal growth breathing with supported coughing strategies to avoid atelectasis, since well-managed technicians reduce discomfort with both physiology and regarded control.
A solid program will educate you to pair these methods with analgesic options when proper. The harmony issues: a small reduction in pain can open motion, and motion can better lower pain. That virtuous cycle underpins improved results after the severe phase.
Documentation that stands up under scrutiny
In the rush, paperwork seems like a task. In truth, it is a safety net and a gift to the next clinician. PUAEME008 emphasizes clear, legible, time-stamped notes. Document baseline vitals, discomfort ranking, and location. Note allergies, current drugs, and the decision path to supply or hold back analgesia. If you administer a medication, include dose, course, lot number when needed, time of management, observed reaction, and damaging effects. For physio therapists, add useful monitorings: helped sit to stand improved from maximum to modest aid after intervention, stride distance raised from 5 to 25 meters, or thoracic development improved by 2 centimeters at the axillary line. Those details make your handover actionable.
Patient interaction and expectation setting
People remember exactly how you made them really feel during pain episodes. Discuss what you are doing, why, and what to anticipate. If using breathed in analgesia, define the beginning, possible negative effects like wooziness, and exactly how you will certainly check them. If you choose not to offer a drug as a result of warnings, say so clearly and describe the plan for urgent referral. That transparency builds trust. For relentless discomfort flare-ups, frame your non-pharmacological approaches as active alternatives, not consolation prizes. Teach tiny, achievable movements that show prompt control. When an individual notices a 20 percent change in pain with breath-coordinated motion, they lean in.
Quality and security culture
The best pain management training programs make safety visible. Tools checks end up being regular. Group briefs go through functions if a client deteriorates. Simulation consists of unusual however critical events such as anaphylaxis or unexpected hypotension. After every circumstance, debriefs explore both technological and non-technical abilities: situational recognition, interaction, and workload management. If your office does not yet have a formal structure for this, bring the routines you learn back to your group and begin tiny. A regular five-minute huddle and a shared stock list are modest steps that stop problems.
Selecting a service provider that matches your needs
Not all courses are equal, and physiotherapists must search for a program that appreciates their range and matches their strengths. Aim for a service provider with skilled instructors from emergency situation, paramedicine, or innovative nursing, that likewise recognize allied health and wellness contexts. Assessment should be real, with observed useful elements, not simply a multiple-choice test. Scenario realistic look issues. Ask if they include documentation drills, handover technique, and non-pharmacological techniques together with pharmacology. Confirm that the discomfort management certificate you obtain states the unit code PUAEME008 and the competencies assessed, considering that this reduces acknowledgment with employers and credentialing bodies.
If your objective is broader than intense care, consider matching PUAEME008 with a longer pain management qualification training course that delves into persistent pain. Lots of physio therapists benefit from that mix: acute stabilization abilities with depth in rehabilitation-oriented pain science.
How the device plays out in day-to-day physiotherapy
Picture a busy musculoskeletal clinic on a Monday. A client shows up blog post ankle joint inversion with swelling and guarded motion. You screen for Ottawa ankle policies, paper weight-bearing status, and determine no red flags. Non-pharmacological procedures bring their discomfort from 8 to 6, but they still can not tolerate talocrural joint assessment. Under procedure and with authority, you provide a short-acting analgesic, display, and within minutes reassess. Currently you can run through cardiovascular test, validate likely grade, supply a functional support, and develop very early loading specifications. The enhanced experience sets the tone, and your plan sticks.
Now change to an area home visit. An older grownup with osteoporotic vertebral fracture is hyperventilating and guarding. You trainer breathing and mild positional modifications, but the discomfort remains serious. You call the duty clinical officer, intensify suitably, and document extensively. Even if you can not carry out analgesia, your PUAEME008 training sharpens your handover, rates care, and keeps the patient safer.
Governance, audit, and the long memory of systems
Any workplace that enables non-medical medical professionals to supply analgesia should have limited governance. That includes controlled storage space, supply settlement, expiry tracking, and case reporting. PUAEME008 strengthens this with practical regimens. The system educates you to track patterns: Are you regularly needing extra dosages for comparable discussions? Are negative impacts clustering at specific times or in particular settings? That feedback loophole causes protocol updates and better end results. In sports programs, for instance, pattern evaluation might change sideline plans for hydration and heat management, which indirectly minimizes discomfort episodes and cramping.
Integrating with more comprehensive discomfort education
If PUAEME008 is your first structured pain monitoring training course, you will likely finish hungry for more. That is the ideal sensation. Sharp pain competence is a foundation. From there, consider programs on relentless discomfort that cover graded electric motor images, discomfort education strategies crafted for different health literacy levels, and pacing techniques that shield function without driving anxiety. Physiotherapists specializing in intricate pain often pursue a discomfort administration accreditation via university-affiliated programs or universities, occasionally stacked as micro-credentials. Those paths match the emergency pain administration emphasis of PUAEME008, offering you a complete range from first-hour like long arc rehabilitation.
Cost, time, and reasonable expectations
Most providers supply PUAEME008 in a one to 2 day layout, with pre-reading to speed the useful work. Expenses differ by area and company, frequently touchdown in an array equivalent to other short courses in pain administration. What matters more than duration is the intensity of simulation and quality of assessment. Anticipate to work through fatigue and obscurity. Anticipate to be observed and to receive direct feedback. If a training course uses a quick certification without sweat, look elsewhere.
Remember that a pain administration certification is the start of your permission journey, not completion. Your employer has to recognize the unit, your scope needs to be documented, and you need to finish workplace inductions specific to medication handling and occurrence management. Maintain copies of all files and guarantee your professional indemnity covers the activities you plan to perform.
A short, useful framework physio therapists can use tomorrow
- Screen fast for red flags, allergies, and current medications, after that choose: analgesia now within scope, or immediate escalation. Pair tiny analgesic gains with precise activity interventions that reveal instant feature change, even if modest. Reassess on the clock: capture vitals and practical markers at pre-set periods, not "whenever." Document as if handing the case to a colleague you appreciate, because you most likely will. Debrief each instance with your team and update local lists if you spot system flaws.
Edge cases and judgment calls
Practice hardly ever follows the manuscript. Clients under-report pain out of stoicism or anxiety of medications. Others over-report out of anxiety or previous adverse experiences. Language barriers make complex scales. Inhaled representatives can cause transient bliss that amazes evaluation, so you must separate influence from analgesia. Rib trauma patients can deteriorate regardless of secure very early vitals. Individuals with chronic opioid usage might not respond to standard dosages, which tempts acceleration that exceeds extent. PUAEME008 does not make these problems vanish. It gives you framework to navigate them without hopeful thinking.
As a physio therapist, your lens continues to be feature. Even in ambiguity, support decisions to whether the person can take a breath, relocate, and secure themselves securely. When uncertain, rise. No certification changes medical humility.
Bringing it all together
Pain monitoring courses help medical professionals react to one of the most human component of their job: suffering. For physio therapists, PUAEME008 Supply pain monitoring includes useful competence in severe situations, strengthens interprofessional language, and boosts the means we connect pain control to activity end results. It does not set you up as a prescriber or pain expert on its own. It does not promise excellence in messy cases. What it provides is disciplined evaluation, much safer instant care, and documentation that respects the following action in the chain.
When you pick a provider, search for scenario-rich training, real assessment, and an educational program that honors your scope. Make use of the discomfort monitoring certification as a bar to enhance regional administration and group routines. After that maintain going. Layer the system with deeper study in consistent discomfort, installed non-pharmacological proficiency, and utilize your special physical rehabilitation skill set to turn quick analgesic home windows right into durable practical gains. That is the job. It is honest, frequently unglamorous, and deeply worthwhile.